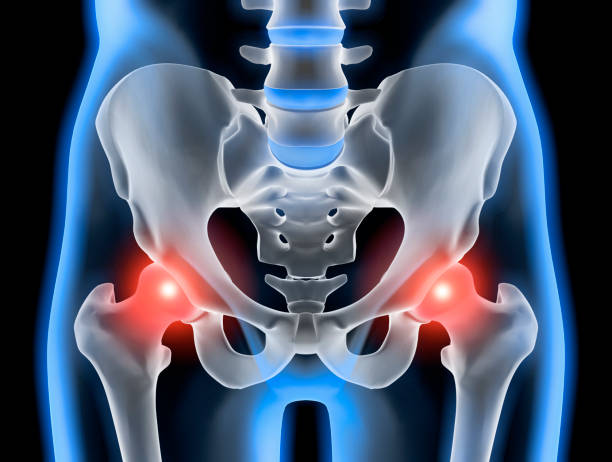
Menopause brings many changes, and one major concern for women is osteoporosis, a condition where bones become weak, brittle, and more prone to fractures. Osteoporosis and menopause are strongly connected due to hormonal changes, especially the drop in estrogen levels that protect bone strength. Understanding how menopause affects bone health can help you take preventive steps early and keep your bones strong and healthy.
In this article, we’ll discuss what osteoporosis is, early warning signs, causes, how menopause increases risk, and how to protect your bones naturally during menopause and beyond.
What is Osteoporosis?
Osteoporosis is a medical condition that causes reduced bone density and increased bone fragility. Over time, bones become porous like a sponge, making them weak and more likely to break, especially in the hip, spine, and wrist.It is often called a “silent disease” because bone loss happens gradually without noticeable symptoms until a fracture occurs.
Key Facts About Osteoporosis:
- Most common in postmenopausal Women
- Bone loss begins earlier but accelerates after Menopause
- Weak bones can lead to fractures, height loss, and reduced mobility
What Are the Early Warning Signs of Osteoporosis?
Early signs are subtle because bone loss happens slowly, but watch for:
- Back pain or discomfort
- Weak grip strength
- Brittle nails and thinning hair
- Receding gums
- Loss of height over time
Causes of Osteoporosis
Osteoporosis can occur due to:
- Hormonal changes (estrogen drop in menopause)
- Aging
- Genetics & family history
- Low calcium and vitamin D intake
- Sedentary lifestyle
- Smoking & alcohol consumption
- Medical conditions (thyroid disorders)
- Low Body Weight / Extreme Dieting
1. Hormonal Changes (Primary Cause in Women)
Estrogen plays a major role in maintaining bone density.When estrogen levels drop sharply during menopause, the body can no longer balance bone breakdown and bone building.Estrogen ↓ = Bone loss ↑Bone starts breaking down faster than it rebuilds.
This is why postmenopausal women are most at risk> Up to 20% of a woman’s bone mass can be lost in the first 5 years after menopause.
2. Aging
As you age:
- Bone-building cells slow down
- Calcium absorption reduces
- Muscles weaken → leading to lower bone stimulation
- Bone becomes thinner and weaker
3. Genetic & Family History
Genetics strongly influence bone health.You’re at higher risk if:
- Osteoporosis runs in your family
- Your mother or grandmother had fractures or height loss
- People with naturally smaller bone frames are also more prone.
4. Low Calcium & Vitamin D Intake
Calcium strengthens bones; Vitamin D helps the body absorb calcium.Insufficient levels lead to:
- Weak bone structure
- Faster bone breakdown
- Poor bone healing
5. Sedentary Lifestyle
Bones need regular movement to stay strong. Lack of exercise causes:
- Muscle loss → weak support for bones
- Reduced bone growth
- Increased bone thinning
- Weight-bearing exercises like walking, dancing, and strength training stimulate bone formation.
6. Smoking & Alcohol Consumption
Smoking
- Reduces estrogen levels
- Slows bone cell activity
- Weakens bone structure
Alcohol
- Impairs calcium absorption
- Affects bone-forming cells
- Increases fall and fracture risk
7. Medical Conditions
Certain illnesses can damage bone health, including:
- Thyroid disorders (hyperthyroidism)
- Rheumatoid arthritis
- Chronic kidney disease
- Cushing’s syndrome
- Malabsorption disorders (Crohn’s, celiac disease)
8. Low Body Weight / Extreme Dieting
Women with low BMI or who did extreme dieting:
- Have lower bone mass reserves
- Lose bone faster
- Higher fracture risk
How Does Menopause Increase the Risk of Osteoporosis?
During menopause, estrogen levels drop sharply. Estrogen protects bone tissue, so when it reduces, bone breakdown happens faster than new bone formation.This is why postmenopausal women lose bone rapidly, especially in the first 5 to 10 years after menopause.
Pathophysiology of Osteoporosis in Menopause
- Estrogen decreases → bone-forming cells (osteoblasts) slow down
- Bone-breaking cells (osteoclasts) become more active
- Net result = rapid bone loss and weaker structure
Rate of Bone Loss After Menopause
Women can lose 2%–5% of bone mass per year in the first 5 years after menopause, then continue losing bone more slowly throughout life.This is why early prevention matters.
How Does Menopause Affect Bone Health?
Menopause impacts bone health by:
- Weakening bone structure
- Increasing fracture risk
- Reducing bone mineral density
- Accelerating natural age-related bone loss
How Do I Know If I Have Osteoporosis?
You may not know without a medical test. See a doctor if you:
- Experience fractures easily
- Have family history of osteoporosis
- Notice sudden height loss
- Bone Density Test (DEXA Scan)
Diagnosing Osteoporosis
Doctors diagnose osteoporosis using:
- DEXA scan (bone density test)
- Blood tests for calcium, vitamin D
- X-rays for fracture evaluation
How to Improve Bone Density During Menopause
To rebuild and strengthen bones:
Lifestyle Steps:
- Resistance training: weights, bands, squats, lunges
- Weight-bearing exercises: brisk walking, dancing, hiking
- Adequate protein to build bone muscle matrix
- Get sunlight exposure for vitamin D production
Foods for Strong Bones:
Milk, yogurt, Cheese, kale, spinach, broccoli, salmon, sardines, nuts, seeds, beans, eggs, whole grains
Supplements
Consult your doctor for:Calcium,Vitamin D3, magnesium, omega-3s
How to Prevent Osteoporosis After Menopause
Osteoporosis is not always avoidable, but you can reduce your risk and protect your bones with lifestyle and dietary habits:
- Increase calcium intake (dairy, leafy greens, fortified foods)
- Supplement vitamin D
- Engage in weight-bearing exercises like walking, jogging, dancing
- Strength training to build bone and muscle strength
- Quit smoking and reduce alcohol intake
- Maintain a healthy body weight
- Eat foods rich in magnesium, zinc, protein, and omega-3 fatty acids
Treatment for Osteoporosis
Treatment may include:
Medical Treatment
- Bisphosphonates (alendronate, risedronate)
- Hormone replacement therapy (HRT) — if suitable
- Calcium & Vitamin D supplements
- Selective estrogen receptor modulators (SERMs)
- Calcitonin or monoclonal antibodies (severe cases)
Common Questions
1. At What Age Does Osteoporosis Usually Start?
Bone loss begins around age 35, but most women notice rapid bone loss after menopause, usually 50+ years.
2. Does Osteoporosis Affect Your Bowel?
Not directly. However, spinal fractures can affect organs, digestion, and posture, indirectly affecting bowel function.
3. Why Is Osteoporosis Called the Silent Disease?
Because bone loss happens quietly without symptoms until fractures occur.
4. Does Osteoporosis Affect Your Nail?
Yes. Brittle nails can be an early sign of calcium and mineral deficiency linked to osteoporosis.
5. What Is the Red Flag for Osteoporosis?
- Sudden back pain
- Loss of height
- Easy fractures
- Seek medical help ASAP if you notice these.
6. What Is the Most Devastating Complication of Osteoporosis?
Hip fractures can lead to disability, loss of mobility, and even life-threatening complications in older women.
Menofix Takeaway
Osteoporosis is serious, but it is not inevitable. With the right steps (nutrition, exercise, supplements, and early screening) menopausal women can maintain strong bones and live healthy, active lives.